In Some Cases, a Sick Economy Can Be a Prescription for Good Health
Conventional wisdom suggests that health improves during good economic times and worsens during tough economic times. When the economy is in recession, stress arising from negative economic outcomes—such as potential job loss, stagnating wages and falling home values—can lead to harmful health outcomes. Similarly, health can be expected to improve when incomes rise and social and psychological hardships diminish. Despite this intuition, recent economic studies suggest the opposite—a recession, as long as it's not too deep or too long, may be good for your health.
Unemployment and Mortality
Economist Christopher J. Ruhm analyzed the relationship between unemployment and mortality rates in the United States over the past few decades. His research shows that when unemployment rates increase, total mortality rates decrease. The effect is economically significant: An increase of one percentage point in the unemployment rate reduces annual fatalities by about 11,000. Why does mortality fall? Ruhm argues that the main reason is that individuals opt for healthier lifestyles during temporary downturns because the cost of leisure time decreases. For example, individuals have more time to prepare healthier meals at home, to engage in physical activity and to visit the doctor. Alcohol and tobacco use is reduced, too, because individuals reduce discretionary spending in periods of unemployment.
On the flip side, fatalities during expansions can increase because of not only lifestyle changes but factors outside of individual behavior. In particular, Ruhm argues that work-related accidents are more likely to occur during periods of expansion,
as individuals work longer hours, and that more-hazardous conditions, such as increased stress, may be more prevalent. Finally, motor vehicle accidents may also
be more common during an economic upturn because improved economic conditions may lead to more traffic on highways and to higher alcohol consumption.
Economists Douglas Miller, Marianne Page, Ann Huff Stevens and Mateusz Filipski took a closer look at the data and analyzed different groups of individuals in terms of age and causes of death. Their results suggest that the most plausible explanation for the negative correlation between unemployment and mortality is not lifestyle changes resulting from reduced work time, nor is it a reduction in work-related stress. The authors find that, among working age individuals, the changes in mortality are related to motor vehicle accidents—there are more accidents (and deaths) during economic upturns, and vice versa. The authors say that their results do not invalidate Ruhm's research; rather, the results help to better understand the mechanisms behind the interaction between unemployment and mortality.
In any case, the strong negative correlation between unemployment and the mortality rate is not in dispute. This phenomenon is not unique to the United States. A similar association has been found in Spain, Germany and other developed countries. However, it is important to emphasize that only temporary downturns or expansions exhibit this behavior. The negative correlation between unemployment and mortality does not seem to hold during periods of sustained or pronounced economic downturns. The current economic downturn, which has been unusually severe by historical standards, may be an example of this. The chart indicates that rising unemployment since 2007 has been accompanied by a recent spike in mortality rates.1
Relationship between Unemployment Rates and Mortality Rates
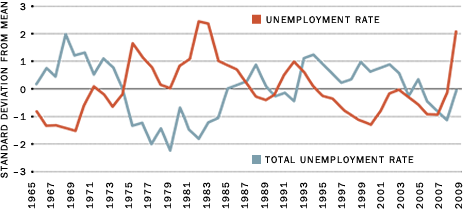
NOTE: Mortality rate data for 2007, 2008 and 2009 are preliminary estimates. The series are de-trended using a linear trend and normalized to have matching scales.
SOURCES: Mortality data are from the Census Bureau's Statistical Abstract of the United States and the National Center for Health Statistics' National Vital Statistics publication. The unemployment data are from the Bureau of Labor Statistics.
Mass Layoffs and Mortality
Job loss typically has lasting economic effects, such as decreases in lifetime earnings and persistent job instability. So, what about the effects of mass layoffs on long-term health outcomes?
Economists Daniel Sullivan and Till von Wachter analyzed a group of workers in Pennsylvania during the 1970s and 1980s and estimated that, for high-seniority male workers, the rate of mortality increased between 50 and 100 percent following a job loss in periods where the employer reduced at least 30 percent of its work force. For example, the authors found that for workers displaced at age 40, the effect over the long term is a decrease of 1 to 1.5 years in life expectancy.2 Across various age groups, workers experienced smaller losses in life expectancy if they were displaced near the retirement age.
The explanation for the higher mortality rate after displacement is that a job loss resulting from mass layoffs produces a decline in lifetime resources, which may lead to reduced investment in health or to chronic stress. A displacement during mass layoffs may also increase the risk of decreased future earnings.
Sullivan and von Wachter note that their results do not necessarily contradict those of Ruhm because high-tenure workers displaced during mass layoffs are different from the average worker who is let go during a recession. For the average worker, temporary declines in economic activity may increase available leisure time for healthy activities, as Ruhm argues, without significantly affecting lifetime resources. But for high-tenure workers, a job loss during a mass layoff entails a significant long-term reduction in earnings, which offsets any benefits from increased leisure time.
The Recent Recession and Medical Care Usage
In contrast to Ruhm's predictions about increasing routine visits to the doctor because of time availability during recessions, another line of research suggests that during the recent economic crisis the effect from the reduced value of time may have been offset by the severe decline in wealth that was observed around the world. Economists Annamaria Lusardi, Daniel Schneider and Peter Tufano document a reduction in individuals' use of routine medical care during the recent crisis in a group of five developed countries: the United States, Great Britain, Canada, France and Germany. They found that the declines were proportional to the out-of-pocket costs that individuals had to bear.3 Lusardi, Schneider and Tufano found that the ranking of countries in terms of privately borne costs for routine care matched the ranking of observed reductions in the use of care. These observations suggest that tighter financial constraints during the recent crisis were the main factor behind the decline in use of medical care.
Endnotes
- It is important to note that the mortality rates for 2007, 2008 and 2009 in the chart are preliminary estimates. [back to text]
- In the study, the authors selected firms that experienced mass layoffs that were not connected to the employees' own health status. In other words, workers were not displaced because they had poor health that made them less productive. This is to isolate the causal effect of displacement on mortality. [back to text]
- The United States is the only country in the group without universal health care coverage. But even in the countries with national health care systems (Great Britain, Canada, France and Germany), individuals incur out-of-pocket costs. [back to text]
References
Lusardi, Annamaria; Schneider, Daniel J.; and Tufano, Peter. "The Economic Crisis and Medical Care Usage." National Bureau of Economic Research (NBER) Working Paper No. 15843, March 2010.
Miller, Douglas L.; Page, Mariane E.; Huff Stevens, Ann; and Filipski, Mateusz. "Why are Recessions Good for Your Health?" American Economic Review, May 2009, Vol. 99, No.2, pp. 122-27.
Ruhm, Christopher J. "Are Recessions Good for Your Health?" Quarterly Journal of Economics, May 2000, Vol. 115, No. 2, pp. 617-50.
Ruhm, Christopher J. "Good Times Make You Sick." Journal of Health Economics, July 2003, Vol. 22, No. 4, pp. 637-58.
Ruhm, Christopher J. "Healthy Living in Hard Times." Journal of Health Economics, March 2005, Vol. 24, No. 2, pp. 341-63.
Sullivan, Daniel; and von Wachter, Till. "Job Displacement and Mortality: An Analysis Using Administrative Data." Quarterly Journal of Economics, August 2009, Vol. 124, No. 3, pp. 1265-1306.
Views expressed in Regional Economist are not necessarily those of the St. Louis Fed or Federal Reserve System.
For the latest insights from our economists and other St. Louis Fed experts, visit On the Economy and subscribe.
Email Us

